 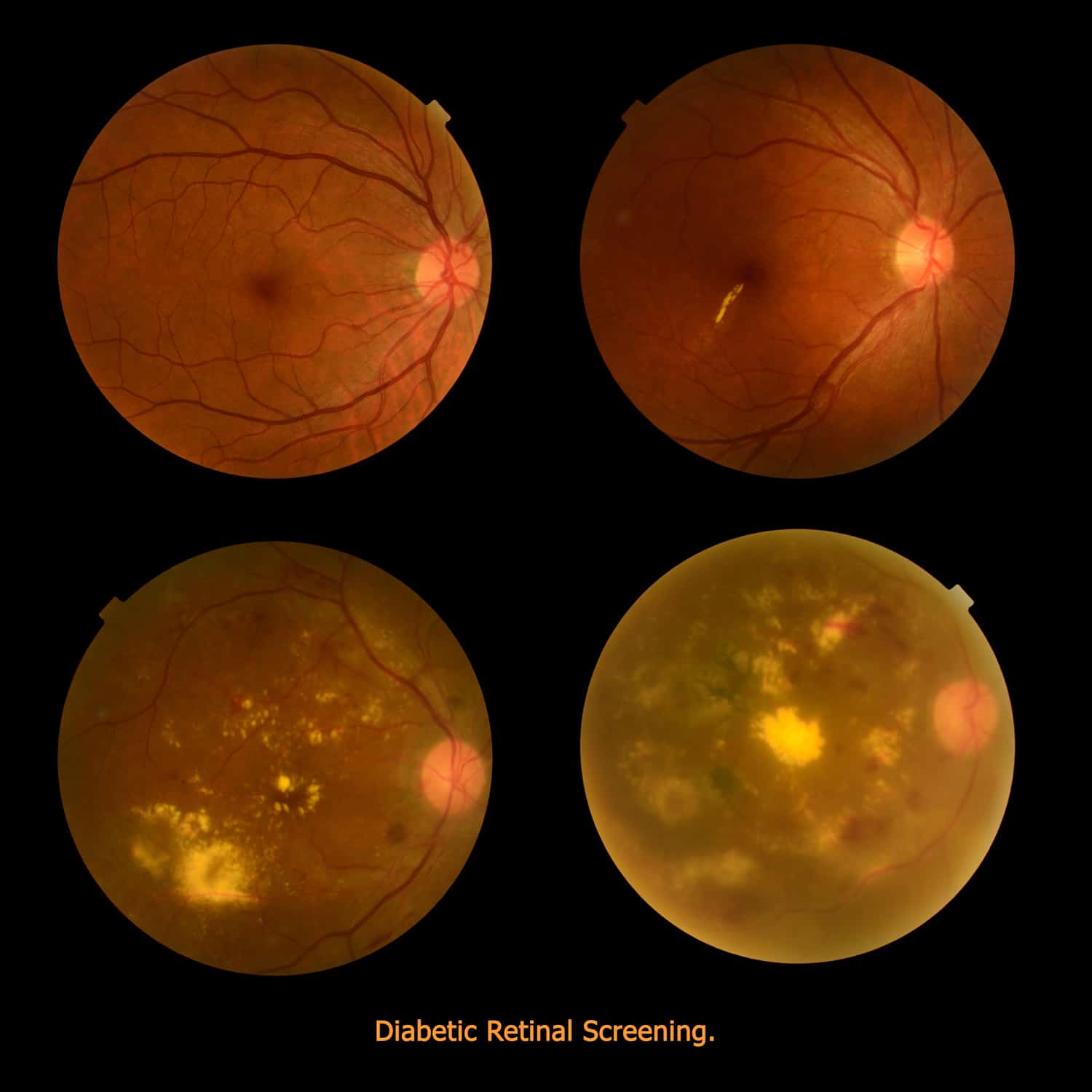
This occurs when there is a break, tear, or hole in the retina. There are three types of retinal detachment: The retina then converts the image to signals that it sends to your brain through the optic nerve. It works with the cornea, lens, and other parts of your eye and brain to produce normal vision. Causes And Types Of Retinal Detachment.Īs written above that the retina is a light-sensitive membrane located at the back of the eye on which when light passes through the eye, the lens focuses an image on your retina. Search up the directory for a Glendale optometrist or search for a Retinal specialist in Glendale, CA. When you notice one or more of these, you should contact an optometrist as fast as possible, to prevent complications and also vision loss. Having a funny heavy feeling in the eye.A sudden vision of floaters, which are small bits of debris that appear as black flecks or strings floating before your eye.Sudden flashes of light upon looking sideways, known as photopsia.However, the presence of the following may indicate a torn retina: Retinal detachment symptoms may not be ominous at first, because it doesn’t present with pain. What Are The Symptoms Of Retinal Detachment? It is an ophthalmological emergency and the longer it goes untreated, the greater the risk of permanent vision loss in the affected eye. Retinal detachment occurs when a thin layer of tissue known as the retina located at the back of the eye pulls away from its normal position. At the same time, traction in the retina or retinal detachments can be corrected.The retina is a light-sensitive membrane located at the back of the eye on which when light passes through the eye, the lens focuses an image on your retina. The surgery can remove scar tissue, blood or fluid, and some of the vitreous gel so light rays can focus properly on the retina. This surgery treats problems with the retina and vitreous, a jellylike substance in the middle of the eye. If you have proliferative diabetic retinopathy, you might need an eye surgery called vitrectomy. Doctors administer both treatments as an injection in the eye. You might also be a candidate for anti-VEGF medication, which can reduce swelling in the macula and improve vision. A steroid injection in the eye can stop inflammation and prevent the formation of new blood vessels. Laser surgery, called photocoagulation, reduces the drive for abnormal blood vessels and swelling in the retina. If you’re in a nonproliferative stage but experience some eye damage, treatment options might include: Your doctor will continue to monitor your eyes, though, to ensure the disease doesn’t progress. If caught very early - before damage to the retina occurs - blood sugar management might be the only necessary treatment. Other treatments will depend on the stage or extent of the disease. Keeping blood sugar within a healthy range can slow the progression of vision loss. This includes taking diabetes medication as directed, watching your diet, and increasing physical activity. Treatment starts with managing blood sugar and diabetes. This triggers different vision problems such as blurriness, reduced field of vision, and even blindness.ĭiabetic retinopathy may lead to irreversible vision loss, but it is treatable. Since these blood vessels are often fragile, there’s a higher risk of fluid leakage. This is an advanced stage of the disease, in which new blood vessels form in the retina. Stage 4: Proliferative diabetic retinopathy At this point, the body receives signals to start growing new blood vessels in the retina. Stage 3: Severe nonproliferative diabetic retinopathyĪ larger section of blood vessels in the retina become blocked, causing a significant decrease in blood flow to this area. This causes an accumulation of blood and other fluids in the macula. Increased swelling of tiny blood vessels starts to interfere with blood flow to the retina, preventing proper nourishment. Stage 2: Moderate nonproliferative diabetic retinopathy This is an area near the center of the retina. Small amounts of fluid can leak into the retina at the stage, triggering swelling of the macula. These areas of swelling are known as micro aneurysms. This is the earliest stage of diabetic retinopathy, characterized by tiny areas of swelling in the blood vessels of the retina. Stage 1: Mild nonproliferative diabetic retinopathy Nonproliferative refers to early stages of the disease, while proliferative is an advanced form of the disease. 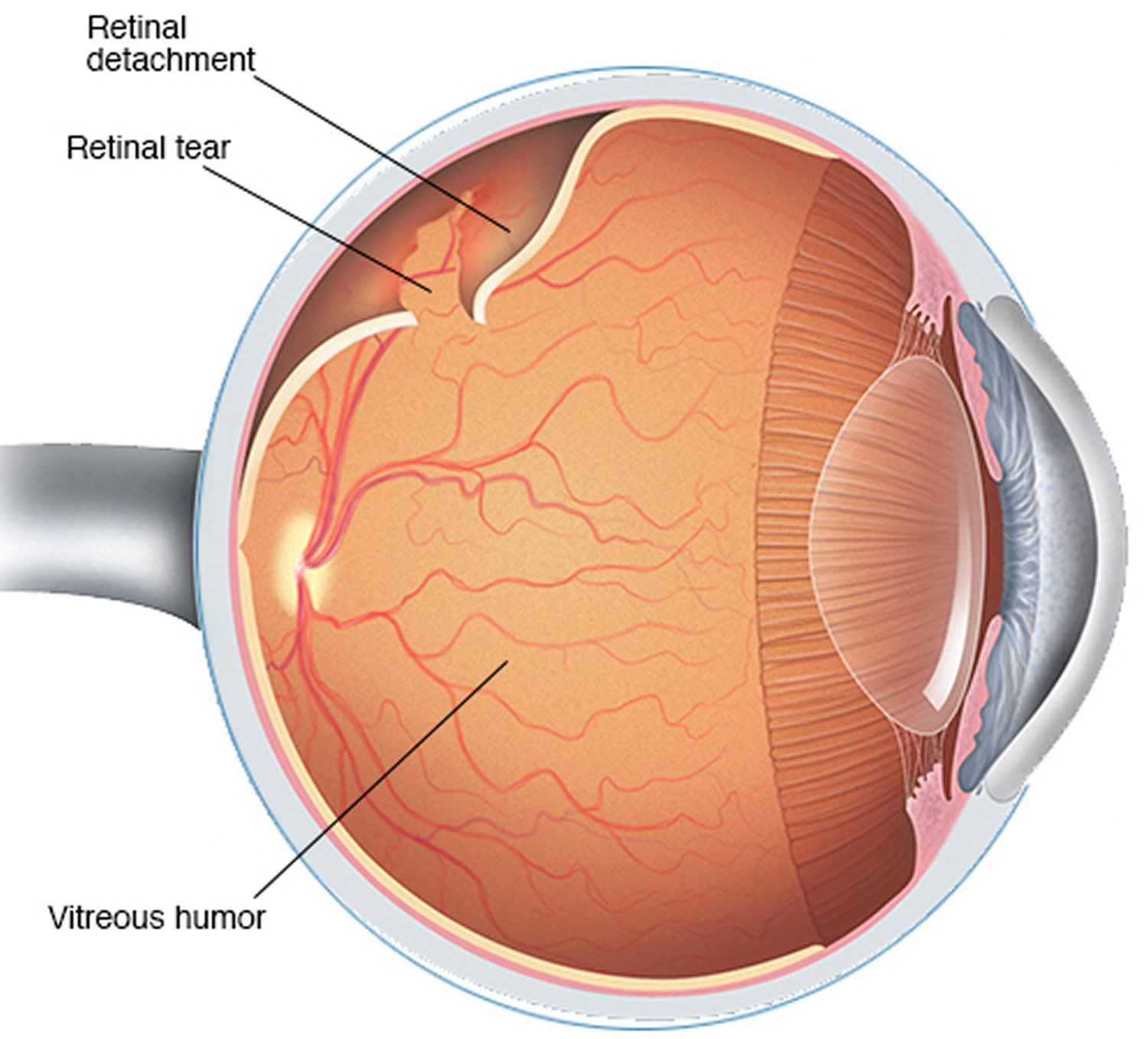
The two types are nonproliferative and proliferative. Diabetic retinopathy is a progressive eye disease classified by two types and four stages. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
